New MRI scanning tech promises to transform healthcare in Kenya
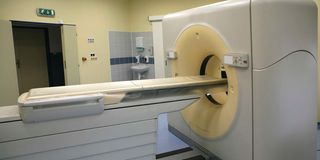
MRI scanners are the cutting edge of medical diagnostics, producing high-resolution images of internal body structures without using radiation.
What you need to know:
- Respiratory illnesses are the leading cause of outpatient visits in Kenya, accounting for 33.8 per cent of all reported cases in 2023, with more than 12 million hospital visits linked to respiratory infections.
A new innovation in medical imaging developed in the UK could soon make life-saving diagnostics accessible to millions of Kenyans, particularly for the respiratory diseases that burden the nation's health system.
Developed through a pioneering collaboration between the University of Sheffield and GE HealthCare, the new low-field Magnetic Resonance Imaging (MRI) scanner leverages artificial intelligence (AI) to deliver high-quality images at a fraction of the cost and infrastructure requirements of conventional machines.
Respiratory disease is the UK’s fourth biggest killer, costing the National Health Service more than £6 billion (Sh1.05 trillion) each year. However, it remains one of the most neglected conditions in terms of advanced diagnostics and treatments.
The new scanner, officially unveiled at the University MRI Unit at Royal Hallamshire Hospital, could change that. It was developed through the EPSRC Prosperity Partnerships programme, which is jointly funded by UKRI's Engineering and Physical Sciences Research Council and Medical Research Council.
Unlike conventional high-field MRI systems, which require large, costly superconducting magnets cooled with liquid helium, the low-field scanner uses recent advances in artificial intelligence (AI) to produce images of a similar quality to those obtained using high-field systems.
Also read: Seeking treatment abroad: The costly journey
By reconstructing low-field scans against thousands of high-field references, the Sheffield-GE team has overcome the long-standing barriers of both image quality and cost. The scanner also incorporates a novel xenon gas imaging technique whereby patients inhale magnetised xenon, making airflow in the lungs visible during the scan and providing detailed insights into lung structure and function.
Highly sensitive and radiation-free, this new technology is safe for patients of all ages, including children. Scans take only a few minutes and can be repeated as often as necessary to track disease progression. A trial involving 60 healthy volunteers is currently underway to establish baseline normative ranges' before moving on to patient studies.
The benefits for patients in the UK are clear: shorter waiting lists, faster diagnoses and the potential for smaller, more affordable scanners to be located in local health centres rather than only in major hospitals.
“Our Low-Field MRI Scanner aims to transform access by making it possible to have significantly smaller, more cost-effective scanners in local health centres. This would bring vital diagnostics closer to patients, speeding up diagnosis and improving outcomes,” said Prof Jim Wild, co-director of the university's Insigneo Institute.
But what does this mean for Kenya?
While the UK stands to save billions on healthcare spending, the impact in countries like Kenya could be transformative.
Respiratory illnesses are already the leading cause of outpatient visits in Kenya, accounting for 33.8 per cent of all reported cases in 2023, with more than 12 million hospital visits linked to respiratory infections, according to the Economic Survey 2025 data by Kenya National Bureau of statistics.
Research also shows that one in four Kenyans with chronic respiratory symptoms faces catastrophic healthcare costs, spending over 10 per cent of their household income on treatment.
At the same time, access to MRIs is limited and centralised. Kenya has just around 50 MRI scanners in total—roughly one per million people—with nearly all of them concentrated in Nairobi and a few other major towns.
Rural communities, where around 70 per cent of Kenyans live, remain underserved. The shortage of specialists further constrains imaging services: the country has just one radiologist per million people, far below the recommended rate of 10 per 100,000.
The cost barrier is also steep. A conventional 1.5T MRI machine costs around Sh70 million. Patients pay between Sh15,000 and Sh50,000 for scans, which is well beyond the means of most families.
The Sheffield-GE low-field scanner addresses many of these challenges. It is more affordable, compact, helium-free and has lighter infrastructure requirements. AI-enhanced imaging reduces the need for a large specialist workforce, and the portable design makes decentralisation feasible, bringing diagnostic capability closer to county hospitals and even community health centres. For countries grappling with widespread respiratory disease and costly diagnostic gaps, this technology could enable earlier detection, reduce out-of-pocket spending and provide more equitable access.
Global potential
The low-field MRI scanner is not just a UK breakthrough—it is a global opportunity. By reducing costs, minimising environmental impact and increasing accessibility, this technology could transform diagnostics in both high-income and low-income settings.
"MRI scanners have been transformative for healthcare, helping medics diagnose a variety of conditions non-invasively. This new low-field technology makes MRI scans easier and cheaper than ever before, enabling more patients to access care and protecting people's health while easing the burden on healthcare systems," noted Lord Vallance, UK Science Minister.
For Kenya and other middle-income countries, this could be the step that bridges decades of inequity in access to advanced medical technology.





