Cervical cancer now leading at Coast referral centre as devolution transforms care
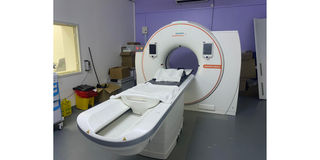
A Magnetic Resonance Imaging machine at the Mombasa Cancer Treatment Centre, located within the Coast General Teaching and Referral Hospital.
What you need to know:
- Cervical cancer tops the list of the cases seen at the facility, followed by breast, esophageal, and prostate cancers.
Since cancer treatment services were devolved from Nairobi to the Coast region, cervical cancer has become the most commonly treated cancer at the region's main referral facility.
At the Cancer Treatment Centre within Coast General Teaching and Referral Hospital in Mombasa, doctors tie the trend to deeper socioeconomic and public health challenges.
Dr Fatma Alamoody, a clinical oncologist who has served at the centre since it opened, says cervical cancer tops the list of the cases seen at the facility, followed by breast, esophageal, and prostate cancers.
“Cervical cancer ranks first in the region. It is especially common in areas with lower socioeconomic activity and high HIV prevalence. I saw the same pattern when I trained in Tanzania,” she explains.
The high numbers, she says, tell a story of women who delay seeking care because of fear, stigma, or the cost of travel and treatment.
The cancer centre was launched in March 2022 under a Ministry of Health programme to devolve cancer care to Mombasa, Nakuru, and Garissa. Many of the first patients treated had been diagnosed years earlier but never made it to Nairobi.
“Before this facility opened, most cancer patients were referred to Nairobi, but only 20 per cent went. Many women could not afford to travel. By the time we started offering services, we were receiving patients who had been referred as far back as 2019,” Dr Alamoody says.
She adds that finances, fear, stigma, and social factors kept many away. Initially, most patients presented with advanced stage three and four disease, limiting survival chances. But increased awareness through media and public sensitisation is beginning to shift that trend.
“We are now seeing more stage one and stage two cases, although the majority still come late,” she notes.
Since 2022, the centre has recorded 6,676 new cancer cases, but the overall workload is far higher: more than 46,000 revisit appointments and over 20,000 treatment sessions.
During that period, 17,158 patients received chemotherapy, 2,782 underwent radiotherapy, and 203 were treated with brachytherapy.
In 2025 alone, the department handled 1,766 new cases and 13,111 revisits, with 4,914 patients on chemotherapy, 1,027 on radiotherapy, and 64 on brachytherapy.
By county, 39 per cent of cases came from Mombasa, followed by Kilifi at 27 per cent, underscoring the heavy regional burden the facility carries.
Though intended to serve the Coast, the centre now receives patients from as far as Kisumu, Machakos, and Mwingi, largely due to shorter waiting times.
While some centres report waiting periods of up to 12 weeks, the Coast facility begins care within two weeks of assessment.
With only one radiotherapy machine initially, the centre handled 65 to 70 patients daily, operating from early morning until late evening. Recently, Dr Alamoody notes, the centre received a new Linear Accelerator, greatly boosting its capacity.
Dr Swabah Ahmed, Mombasa Heath executive, explains how the centre is coping with rising demand.
“A second radiotherapy machine is a huge step forward. With just one, we were treating about 50 patients daily from Kilifi, Kwale, and as far as Machakos. It was strenuous. Now, with the new machine, we can treat up to 140 patients a day, which is a huge boost in our fight against cancer.”
Dr Alamoody adds: “Now that we’ve added the second machine, I envision the number going even higher. This allows patients to start treatment sooner and reduces the long waits they faced before.”
Each radiotherapy session lasts 15 to 20 minutes, but treatment may continue for up to seven weeks, depending on the type and stage of cancer.
Radiotherapist Carson Ng'etich, who gave the Nation a tour of the centre, explains the process: treatment begins with imaging the cancer using MRI. The results go to the planning unit, where the tumour is mapped to determine how to deliver radiation precisely, minimising impact on surrounding healthy tissue.
“The radiotherapy machine, combined with careful planning, ensures we treat only the targeted area. We protect the patient to prevent harm from radiation. Even in cervical cancer, where we use brachytherapy — internal radiation — the process is carefully controlled. If I enter the points into the machine and notice any part lies outside the tumour outline, I cannot start the radiation,” he says.
Patients no longer need to travel to Nairobi for radiotherapy, chemotherapy, or specialised oncology care.
“All treatment is available here now,” says Dr Alamoody. “Being at the main referral facility makes it easier for patients to access care.”
The centre offers screening, chemotherapy, radiotherapy, brachytherapy, surgery, and palliative care. However, PET scan imaging, critical for confirming whether cancer has been fully cleared, remains unavailable locally. Despite this, the centre has already formed a cancer survivors' group, a sign, doctors say, that outcomes are improving.
“Of seven patients I recently sent for PET scans, five came back clear,” Dr Alamoody reveals.
Challenges
Even as access improves, significant challenges remain. The chemotherapy unit is small and overstretched as patient numbers grow. Staffing needs to expand, and funding gaps threaten sustainability. Most patients rely on SHA coverage, but treatment limits are often exhausted mid-course, forcing difficult decisions.
“The SHA allocation was about Sh500,000, which gets used up very quickly due to the high cost of treatment. The government had promised to increase it to Sh800,000, but that has not yet taken effect. Additionally, delayed payments at times strain the running of our activities here,” says Dr Alamoody.
She adds that blood shortages remain another critical hurdle, with some patients forced to interrupt treatment for weeks while waiting for transfusions.
To patients, Dr Alamoody has a clear message: seek help early and do not fear the diagnosis.
“Cancer is treatable, especially when caught early. We are here to help,” she says.
For policymakers, she urges prioritisation of cancer care, noting the disease now affects nearly every household. “Everyone has a story. It is no longer about a neighbour; it is in our homes. We must treat it as a priority.”
As cervical cancer continues to lead at the Coast, health experts emphasise that screening, vaccination, lifestyle changes, and early diagnosis remain the strongest weapons in reducing the burden.





