One nurse, nine babies: Neonatal units operating at up to five times recommended ratios
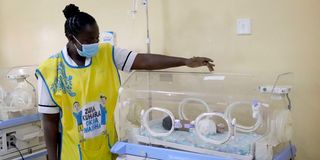
A nurse checks on newborns in incubators at Homa Bay Teaching and Referral Hospital’s maternity ward.
On a busy night shift in a Kenyan public hospital, a single nurse walks between rows of incubators and cots. Some babies are on oxygen. Others require intravenous medication. She cannot be everywhere, there are too many babies and only one of her.
Collins Ajwang, President of the National Nurses Association of Kenya, does not mince words about what the workload looks like on the ground.
"In a busy ward round, a nurse attends to over 15 children. There is so little she can do," he says.
New research presented at the International Maternal New-born Health Conference (IMNHC) 2026 in Nairobi has put hard numbers to what nurses on the ground have been saying for years.
In neonatal units across Kenya, Malawi, Nigeria and Tanzania, nurses are able to complete only one-third of the care tasks that new-borns require. One third is delegated to mothers and unsupervised nursing students who have no medical knowledge to look after sick children, and one third is missed entirely.
The international standard is that no nurse should be responsible for more than two children at any one time in the wards. In Kenya, the reality is radically different.
"The most a nurse should take care of at a given time is two children, but that is not the practice in Kenya. We take care of even seven children or more in a session. With that ratio, not all can have quality care. Something needs to be done," Ajwang tells Nation.
The data, from research by NEST360, was presented at the Nairobi conference last week. Dr Abdulazeez Imam, Assistant Clinical Professor at the London School of Hygiene and Tropical Medicine, described what it showed about intravenous medication administration in particular.
"When we looked further at the data, we saw nurses almost always handed over patients and did clinical assessments before shifts. Sometimes they were involved in intravenous medication, which was also delegated to students. They rarely did vital signs, which was largely a student role. They rarely cleaned the baby or changed diapers, this was almost always delegated to families," he said.
The numbers on IV medication are particularly alarming. Four in every ten intravenous medications in neonatal units were administered by nursing students with minimal supervision, and one in ten was missed altogether. In a setting where a baby weighing 700 grams requires medication calculated to the nearest decimal point and routinely double and triple-checked by trained clinicians, those figures represent a serious and ongoing risk to infant lives.
"A small and sick new-born who weighs 700 grams needs a very small volume of medication. You need to calculate that diligently, and it is usually double and triple-checked," Dr Imam said. "We noted that four in 10 IV medications were given by nursing students who had minimal supervision. This is a risk to the infants."
Alice Tarus of NEST360 laid out the staffing numbers behind these failures. In a standard 12-hour shift, the median nurse-to-baby ratio across the facilities studied was one nurse to nine babies, against an international standard of one nurse for every two babies requiring serious attention and one nurse for every four stable babies. Kenya and its neighbours are working at roughly four to five times the recommended ratio for the sickest infants.
"For a 40-bed unit at 100 per cent occupancy, with 10 beds for complex cases and 30 for stable babies, we tried to cost what it would take per shift to meet recommended standards," Ms Tarus said.
For Malawi alone, the analysis found that between 300 and 400 additional nurses would be needed across 37 hospitals to meet recommended staffing levels. Hiring general nurses to close that gap would cost approximately US$3 million annually, while bringing in specialised neonatal nurses would cost closer to US$8 million per year, before accounting for training costs of approximately US$9,000 per hospital to establish on-site, simulation-based learning programmes.
"Clearly, it calls for more financing," Tarus said.
Beyond the immediate clinical risks, the NEST360 research also captured what sustained pressure at this level does to the nurses themselves. One nurse, interviewed as part of the study, described her experience after additional nurses were deployed to her neonatal unit.
"I did not go on leave for almost two and a half years. At least when they came, we now take at least a break to rejuvenate ourselves," she said.
Dr Imam said burnt-out nurses cannot provide quality care. "They make more errors. They disengage. They leave the profession or leave the country."
Kenya is already experiencing significant nurse emigration as better-paid opportunities in the United Kingdom, the Middle East and elsewhere draw trained professionals away from a public health system that cannot match those salaries.
"The nurses in Kenya's new-born units are not failing their patients. They are working within a system that has failed them, failed to hire enough of them, failed to pay them enough to stay, failed to relieve them of workloads that would break anyone, and failed to protect them from the moral injury of knowing that the care they are delivering falls short of what those babies and those mothers deserve," Ajwang says.
He adds that babies in Kenya's neonatal units need one nurse for every two of them when critically ill, yet they are getting one nurse for every nine.
The study recommends increasing the number of general nurses and training them on-site, so that the few skilled nurses already in post are not pulled away for off-site training, and establishing a government-sponsored diploma in neonatal nursing as a defined career pathway. It points to Ethiopia, which has already begun building this specialised cadre, as a model to replicate.
It also calls for improved pay and working conditions, investment in equipment, and specific planning for night shifts, which are consistently the most dangerous period in any neonatal unit because staffing drops and oversight thins.
"We have to acknowledge that nurses are moving out of the country, so paying them more, motivating them and system planning, we cannot leave that behind," Tarus said.
The National Nurses Association of Kenya has called for an urgent review of nurse-to-patient ratios, increased recruitment, better pay and improved working conditions. The response from the system, Ajwang says, has been slow.