Prof Faith Osier: The Kenyan scientist bringing vaccine manufacturing closer home

Prof Faith Osier, a Kenyan scientist based in the UK. She leads Chanjo Hub, which aims to expand vaccine manufacturing capacity across Africa and has an initial focus on Kenya.
What you need to know:
- In Kenya, Prof Osier is currently piloting a new malaria vaccine using messenger RNA (mRNA) technology.
- In Ghana, her team is using chicken and quail eggs to develop new life-saving vaccines.
Three years before the first-ever malaria vaccine was officially approved by the World Health Organization, Prof Faith Osier delivered an inspiring seven-minute TED talk about how close the world was to having one.
That video appears whenever you search her name online besides her designation as an immunologist, paediatrician, and educator.
She stood on the dimly lit stage with just her microphone, inspiring the world with a vision that was not yet realised, but she was hopeful it was near.
At the time, her team was working to understand the malaria-causing parasite Plasmodium falciparum in order to develop a suitable vaccine candidate.
“We did this in Africa, and we are very proud of that,” she declared, as the audience cheered.
She was right. In 2021, the world got the first-ever malaria vaccine, which is given to children under the age of five, and Kenya was one of the first countries to roll it out.
Around the time of the vaccine’s approval, the world was dealing with the Covid-19 pandemic, one that laid bare the inequities that exist across the globe.
“Vaccines were being made in high-income countries. These countries focused on supplies for their own populations. Commitments made to donate vaccine supplies to Africa were mostly not met,” she tells Healthy Nation in an interview.
“The wake-up call was that Africa needed to become self-sufficient and be able to supply vaccines for the continent,” she adds.
It was then that Prof Osier’s idea for Chanjo Hub, an Africa-led vaccine manufacturing initiative, was born. Chanjo Hub is funded by the Department of Health and Social Care as part of the UK Vaccine Network, a UK Aid programme to develop vaccines for diseases with epidemic potential in low- and middle-income countries.
Prof Osier is a professor of Immunology and Vaccinology in the department of Life Sciences and is co-director of the School of Convergence Science for Health and Technology at Imperial College London.
"We designed a project focused on small-scale manufacturing because it was a university-led initiative,” she explains.
She began the project in two countries: Kenya and Ghana.
In Kenya, she is currently piloting a new malaria vaccine using messenger RNA (mRNA) technology. In Ghana, her team is using chicken and quail eggs to develop new life-saving vaccines.
The mRNA technology involves a genetic code that provides a ready-made protein, enabling the body to produce antibodies and trigger an immune response upon infection.
“We chose these technologies deliberately because we are able to do it in a small space and in a more cost effective manner. You don't need a huge factory.”
In Kenya, Prof Osier is partnering with Tasa Pharma, a local pharmaceutical company recommended by the government due to its sterile manufacturing facility.
The Kenya BioVax Institute, the government’s flagship vaccine manufacturing initiative, had only been established the same year Prof Osier conceived the idea, but they are now collaborating, along with the Kenya Medical Research Institute.
Prof Osier and her team are currently in the pilot phase, conducting tests in the United Kingdom, where the necessary technology is readily available. Her goal is to transfer that technology to Africa so local scientists can manufacture vaccines from scratch.
“Later this year (2026), we will be in a position to begin the technology transfer to Kenya BioVax and Tasa Pharma so that by the end, we can transfer the capability for the entire process,” she says.
Prof Osier explains that the malaria vaccine her team is developing is slightly different from the existing one in a key way: it acts at a different stage of a malaria infection.
“The current vaccine works on the sporozoite stage; the stage when a mosquito bites you. It tries to block the development of that sporozoite. From there, the parasite moves to the liver, and once it exits the liver, it enters the blood stage. It is the blood stage that makes you sick,” she explains.
“What our vaccine does is work on the blood stage. If the parasite escapes, our vaccine induces immunity that acts at the blood stage,” she adds.
Prof Osier chose to focus on a malaria vaccine for Kenya because she has been working in this field since 1998 after collaborating with researchers from the UK who were based in Kenya at the time.
“I started working in Kilifi as a junior doctor many years ago, and I was so surprised by how malaria was making young children sick, and how they were dying. I grew up in Nairobi and had not seen the impact of malaria firsthand,” she shares.
In Ghana, the team has a similar arrangement, this time with a partner in the United States.
The US-based partner is training them in egg-based vaccine development, beginning with production in the US before transferring the technology to their Ghanaian partner, the Council for Scientific and Industrial Research.
At this initial stage, her team is also mapping the potential cost of the vaccine, assessing its acceptability among the population, and evaluating the regulatory environment, given the strict requirements for health products.
South Africa has since become the third country to join the Chanjo Hub. In their context, they are using a plant scientifically known as Nicotiana benthamiana to come up with new vaccines that can be used for Human Papilloma Virus and the Rift Valley Fever.
What next after the pilot phase?
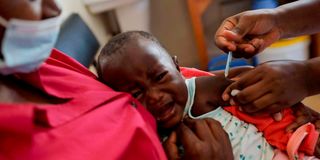
A nurse administers a malaria vaccine to an infant at Lumumba Sub-County Hospital in Kisumu.
If Prof Osier and her team succeed in developing a viable product, the next step will be clinical trials. This will mean giving real people the vaccines to see if they actually work.
“If that will be successful, then it would really give us the energy to produce it on a much larger scale,” she says.
“The aim of the project was really to build the capacity to manufacture vaccines locally. We want people trained so that if we can produce a malaria vaccine, we can also make vaccines for other diseases that are problematic in Kenya,” she adds.
Social media has become awash with misinformation, particularly around childhood immunisation. Prof Osier urges everyone to always verify their sources and seek advice from health practitioners rather than relying on social media.
“Once it hits you, you will know. When you see a child with measles or treat a child who has died from malaria, and you see what they go through yet that could have been prevented by just getting a vaccine, it will not be hard to be convinced,” she says.
Prof Osier also reminds young scientists in Kenya and beyond that they each have a role to play in development.
“If we can play our part and improve the health of our people using the knowledge we have gained, then we should do so,” she says.