
A section of health workers employed under the Universal Health Coverage (UHC) programme protest outside the National Treasury Building in Nairobi on May 27, 2025.
As Kenya enters 2026, the healthcare sector is undergoing a high-stakes transition marked by reform pressures, labour unrest and heightened international scrutiny.
The shift from the National Hospital Insurance Fund (NHIF) to the Social Health Authority (SHA) is complete, but the new system faces early stress tests that will determine the future of Universal Health Coverage (UHC).

Social Health Authority (SHA) officials during a registration exercise at Nyayo Gardens in Nakuru on July 23, 2025.
The year opens with policymakers grappling with competing priorities: stabilising the SHA, managing a restive health workforce, navigating a suspended US-backed health partnership and operating within a tightening fiscal environment.
At the centre of the reform agenda is the operational maturity of the SHA. By the end of 2025, registration had reached 19.3 million Kenyans, shifting focus from enrolment to access. A major challenge remains the means-testing model used to assess contributions for informal sector workers.
Millions are registered but unable to fully access benefits due to delays and assessment bottlenecks, exposing the system to growing public frustration.
Private and faith-based hospitals, which deliver nearly half of Kenya’s clinical services, have also expressed concern over reimbursement delays, fearing a return to the debt accumulation that strained facilities under the NHIF.
Referral hospitals say they are overwhelmed as patients bypass primary healthcare facilities, where services are free, and head directly to higher-level hospitals. Administrators argue that this behaviour strains specialist staff and resources meant for complex cases.
This pressure came into sharp focus in November when more than 100 women were detained at Mama Lucy Kibaki Hospital over unpaid medical bills. Hospital chief executive Frederick Obwanda attributed the crisis to low uptake of social health insurance, saying hospitals are forced to demand cash payments for sustainability.

Mama Lucy Kibaki Hospital in Nairobi.
He said counties have invested in staffing and drug supplies at lower-level facilities, but patient preference for referral hospitals undermines efficiency and inflates healthcare costs. Mr Obwanda argued that enforcing the referral system would ease congestion at major hospitals and allow specialised facilities to focus on complicated cases.
Kenyatta National Hospital chief executive Dr Richard Lesiyampe echoed these concerns, noting a surge in routine cases at the national referral facility. He said KNH is handling unusually high numbers of normal deliveries, stretching staff and supplies, despite the existence of adequately equipped lower-level hospitals. While the referral framework exists, he noted, enforcement and compliance remain weak.
Health worker migration
Beyond financing and patient flow, labour relations remain the sector’s most volatile fault line. Kenya continues to face a severe shortage of health workers, producing about 7,000 professionals annually against an estimated deficit of 70,000 required to meet global standards.
The most contentious issue heading into 2026 is the fate of more than 8,500 UHC staff hired on short-term contracts during the Covid-19 pandemic. Their demand for permanent and pensionable terms remains unresolved, fuelling strike threats across the sector.
Clinical officers, including interns, went on strike from December 22, 2025, citing repeated failures by the Ministry of Health and county governments to honour agreements, court orders and government directives.

The Social Health Authority building in Nairobi.
Kenya Union of Clinical Officers national chairman Peterson Wachira said the dispute centres on unresolved legal and financial commitments, including stalled collective bargaining agreements (CBAs), delayed salary reviews and failure to absorb contract staff.
Despite court directives and internal agreements to conclude CBAs by December 2024, progress has stalled. While the Ministry of Health’s CBA is reportedly finalised and awaiting signing, negotiations at the county level have been delayed for more than a year.
Mr Wachira said county governments have ignored advice from the Salaries and Remuneration Commission to implement the third and fourth phases of salary adjustments, despite formal communication in 2024.
He added that court-backed return-to-work agreements requiring promotions, staff absorption and recruitment remain partially implemented, with only a few counties complying.
Delayed absorption of UHC and Global Fund staff remains one of the union’s biggest grievances. Mr Wachira said affected workers have gone unpaid for more than a year despite budgetary provisions and directives from the Labour Relations Court, Parliament and the President. He warned that industrial action has become the default tool for securing reforms, reflecting the failure of structured negotiations.
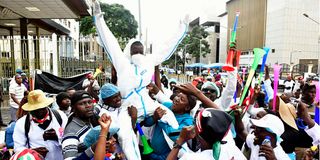
Universal Health Coverage (UHC) workers protest outside the National Treasury Building in Nairobi on May 27, 2025.
Beyond labour unrest, Kenya is also grappling with a growing health worker migration crisis. A TruMerit report released in early 2025 ranked Kenya as Africa’s leading source of nurses migrating to the United States.
Kenyans accounted for 6.5 per cent of African applicants seeking US VisaScreen certification, placing the country third globally after the Philippines and Canada. Nigeria and Ghana followed at five per cent and four per cent respectively.
The exodus has been driven by limited funding for public healthcare, poor working conditions, long hours and low pay, even as many trained nurses remain unemployed or underemployed locally.
On the diplomatic front, the sector has been further complicated by the Kenya–US Health Framework, a five-year $2.5 billion government-to-government agreement intended to replace donor funding through NGOs.
Under the deal, the US would provide up to $1.6 billion directly to Kenyan institutions, including the SHA, Kenya Medical Supplies Agency and the Digital Health Agency, supporting programmes on HIV/AIDS, tuberculosis, malaria, maternal and child health, polio eradication and disease surveillance.
However, the agreement was suspended on December 19, 2025, after the High Court issued conservatory orders following petitions by Senator Okiya Omtatah and the Consumer Federation of Kenya. Justice Chacha Mwita cited lack of public participation and parliamentary approval.

US Secretary of State Marco Rubio and Kenyan Foreign Cabinet Secretary Musalia Mudavadi sign the US-Kenya health pact as President William Ruto looks on.
Critics warned of potential US access to sensitive medical and genomic data, concerns the government dismissed, insisting that only de-identified, aggregated data would be shared in line with the Data Protection Act (2019) and the Digital Health Act (2023).
With the suspension in place, the health sector now awaits clarity on whether the partnership will proceed and how its delay could affect funding for critical programmes.
Ultimately, the defining test for 2026 will be the government’s Primary Healthcare pivot. The State has deployed 100,000 Community Health Promoters to deliver preventive care at household level, aiming to reduce pressure on hospitals and protect the financial sustainability of the SHA.
If the model succeeds in linking households to dispensaries and detecting illness early, 2026 could mark a turning point for Universal Health Coverage. Failure, however, risks pulling the sector back into the familiar cycle of debt, strikes and reform fatigue that has plagued it for more than a decade.










