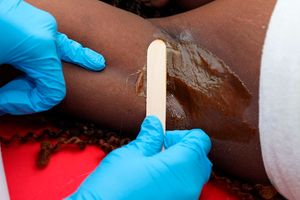
In many societies, talking about what the genitalia looks like is still taboo; hence, many women would not know what another woman’s looks like.
She called it the best decision she had ever made as a woman. “Yet I can’t tell my mother. If she knew that three of her daughters, each paid about Sh250,000 for clitoris reconstruction surgery, she’d very disturbed.”
The 32-year-old woman, who asked to be identified only by Safia, grew up in Nairobi. She underwent female circumcision, often called female genital mutilation or ‘cutting’ (FGM), at the age of nine.
“We never knew then that female circumcision was a bad thing; it was a sense of cultural pride. In my family, when girls reached nine years, they’d travel from Nairobi to the village to get circumcised. They’d come back with gifts. So it’s something I looked forward to. Many girls did. But when my turn came, my mom and aunts decided my two cousins and I would get circumcised in a clinic in Nairobi because one of my five sisters almost lost her life because of an infection,” she says.
“I can’t remember feeling pain. My healing was fast; perhaps my anticipation of finally being ushered into womanhood, and receiving gifts, made it feel that way.”
Unlike her sisters, Safia was given painkillers and antibiotics after the cut. “I didn’t get to experience the pain and trauma that I hear of about FGM,” she tells Nation Lifestyle.
Sexual function
Being circumcised never really bothered her, particularly in terms of sexual function, until her elder sister did a clitoris reconstruction or restoration, a procedure known as clitoroplasty.
“I studied in Nairobi, yet it never crossed my mind that I was different. But my mom also made us not talk about it. It was hush-hush, so it’s not something I discussed. But when I joined a national secondary school, I got to interact with children from many backgrounds. And that’s the first time I heard the word FGM. It was introduced as a bad thing. I wondered, ‘what are these people talking about? Why is it wrong?’ But when I reached Form 3, that’s when I realised, okay, everyone around me hadn’t done it. This is not right. My mom did something wrong. Our culture does something wrong. It shouldn’t happen,” she says.
When she started dating her partner, she told him about the cut, but not out of shame.
“I was still proud of my culture; he’s not from my community, but he wasn’t put off. Our sex life was okay. But what I really wanted to understand was how the cut had impacted my ability to have children. I had read a lot about how women who’d undergone FGM had complications during childbirth. I grew up in a home—like in many Somali households—where sex and anything related to that part of the body wasn’t talked about.
So, when I got pregnant, I kept nagging my gynaecologist, ‘will it impact me?’ He eventually had to physically examine me to assure me that I’d be fine and could have a vaginal birth. My sister had experienced so many complications, and that really haunted me. But in the end, I delivered my babies naturally, without any complications.”
Having seen the woes caused by FGM, Safia’s eldest sister was the first to think about reconstruction surgery.
“After having three children and seeing what FGM had done to her, she started reconsidering clitoral repair. For her, sex was performative; she never experienced pleasure; it hurt. She found a doctor who was doing pro bono work among marginalised communities,” she says. “After my sister’s surgery, we started seeing the possibility that we could be repaired. A second sister did the surgery, but by a plastic surgeon. As a woman, the older you get, the more you want to live your life to the fullest and when my sisters told me, I was like okay, I want to do it. Every new year, I'd say ‘this year’. But when a friend, someone I’m more open with, did the surgery and said she was experiencing things she’d never experienced, I knew for certain it was a matter of time,” says Safia.
The results of clitoral reconstruction or restoration are not the same for everyone; they depend on the severity of the cut or mutilation. Unlike other Kenyan communities that cut, sewed and closed all or part of a girl’s external genitals, it was only Safia’s clitoris that was nipped. Therefore, it was not so hard for the surgeon to uncover Safia’s remnant of the clitoris beneath the scar, unlike her sister’s.
“The plastic surgeon explained that my skin was very sensitive and paper-thin. But luckily, my labia majora and minora had not been severed. I believe the nurse showed some mercy in my case because she did not cut everything. For my sisters, however, the traditional medicine woman cut everything and stitched it closed. The surgeon worked with the tissue that was still present and pulled it outward. He did not add skin from anywhere else,” she says.
However, in the US, some plastic surgeons pick skin from inside the cheek and graft it over the clitoris and use fat from the stomach to reconstruct badly mutilated women’s private parts.

Marsabit girls who underwent medicalised FGM.
Safia says the healing was smooth.
“Peeing wasn’t painful. But something happened to me during my healing. As Muslims, we use bidets to wash ourselves. The first week, I had a bandage covering my privates, so I’d just pour water using a jug. But once the bandage came off, instead of listening to my doctor, I asked my sister, who’d had the procedure before me. What I didn’t realise was that the water pressure in her toilet was much lower than mine. When I used the bidet, one of the stitches came loose. I felt like something was dangling, and I panicked. I went back to the doctor, and he stitched it again. Thank God it hadn’t caused any major damage.”
After the reconstructive surgery, Safia, her sisters and five friends have since seen the benefits.
“The sensitivity is higher. Before the reconstruction, when I was intimate with my husband, I felt something. But I’ve come to realise that it was only like 40 per cent of it. When the bandage got off about five days after the surgery, I’d sit or even wear pants or jeans and start feeling sensations I’d never felt before. I felt awkward. For the first time, I felt something between my legs and involuntary pulses. It felt like a weird foreign object the first few days, but now I’m getting used to it.”
In many societies, talking about what the genitalia looks like is still taboo; hence, many women would not know what another woman’s looks like. Was she ever curious? Has the enhanced sexual function made her feel more normal?
“I was curious when I got older, but I never asked. I wouldn’t know what other women look like, but now I feel normal, my parts are visible.”
Safia says she chose a plastic surgeon because she wanted more than just repair.
“A plastic surgeon pulls and increases the surface area, because it’s like the more surface area, the more nerves that are exposed, the more pleasure. And it’s not only the sensations; it is how that body part now changes during arousal. Previously, intimacy was more mental; now it is more physical. Nowadays, it even lasts longer. Maybe this feeling isn’t unique and is normal for many women, but I’m happy,” she says.
Doctors advise a few weeks off intimacy for proper healing.
“After the numbness goes away, there’s a bit of discomfort, but it wasn’t like I had gone through a major surgery to stop me from my day-to-day life. Immediately after the bandage came out, I started feeling like there was a whole new system, it’s like buying a new car… By week two, I was counting days, but I was given the go-ahead eight weeks after the surgery,” she says.
The cost?
“Sh200,000,” she says, “My partner actually paid because it’s something he knew I wanted. We usually plan for our finances, and I’d always talk about how I wanted to set aside money for the surgery. Then one day, he said, ‘Why don’t you go do it? If you’ve really thought about it.’ I said, ‘It’s expensive. I need to put money aside.’ He said, ‘I'll pay for you.’ And I’m so grateful.”
Clitoral restoration
Safia says she believes many women are doing the surgery to restore their sexual function, but it is rarely talked about openly.
“People do not give interviews or speak about it in public. Personally, I know about six women who have done it, but I believe the number is much higher. My referral chain includes me, my sister and my friends, through whom other women have also been referred. In fact, one of my closest friends went through the procedure just three weeks ago,” Safia says.
“If I were to advise any woman who’s undergone FGM and is in a position to do the reconstructive surgery, do it. You get to experience intimacy on another level that you will probably not experience because of a cultural practice someone else decided for you.”
The World Health Organisation says that while there are some promising reports that clitoral reconstruction or restoration may relieve pain, there is not yet enough evidence of safety and effectiveness. The organisation advises against raising unrealistic expectations, especially for women seeking sexual improvement.
Still, demand for such operations is growing. A substantial number of Kenyan women have undergone female genital cutting, and it was only recently, when they reached their 50s, 40s and 30s, that they discovered this new medical procedure.
Dr Christopher Matwa is among the few medical professionals in Kenya who are doing these genital reconstruction procedures.
“I come from a community where FGM is rampant. Growing up, we didn’t know it was wrong or that it was a medical problem. It wasn’t until these campaigns like ‘Stop FGM’ came that we learned that it is a harmful practice,” says the plastic, reconstruction and aesthetic surgeon.
His path to reconstruction surgery did not start with FGM cases, but with difficult wounds he encountered as a medical intern—diabetic ulcers, venous ulcers, and other injuries that refused to heal.
“We were often helpless. Even our superiors did not always know how to deal with such wounds,” he says.
That early exposure sparked a fascination with tissue repair and restoration, eventually leading him to study plastic, reconstructive and aesthetic surgery at the University of Nairobi.
“The goal wasn’t FGM reconstruction at first. But when I began studying plastic surgery, I realised the field was wide. It also includes clitoroplasty.”

Plastic surgeon Dr Christopher Matwa during the interview at his office in Nairobi on November 24, 2025.
Cultural belonging vs personal well-being
The immediate physical risks of FGM include excessive bleeding, infection, difficulty healing and extensive scarring. Many procedures are done in non-sterile conditions, increasing the likelihood of complications. But Dr Matwa emphasises that the effects of FGM extend far beyond visible injury.
“It’s not just physical, it’s social and emotional. When it heals, the scar tissue is often left looking and feeling irregular,” he says. But the emotional and social consequences are often the most difficult to navigate.
“In their culture, girls who’ve undergone FGM may fit in perfectly. But once they leave that environment, fitting in becomes a problem. Such a girl may not be comfortable with friends or partners. She feels she isn’t normal,” he tells Nation Lifestyle.
That internal conflict between cultural belonging and personal well-being is often the strongest driver behind women seeking reconstruction later in life.
The surgery depends on the type of FGM. There are four recognised types, ranging from partial cutting to extensive removal of the external anatomy. An initial assessment of the woman is what determines what is medically possible and how complex the procedure is likely to be.
“Types one and two affect mainly the clitoris. Types three and four are more severe,” says Dr Matwa.
With mild forms of FGM, reconstruction is less complex. With advanced forms, significant tissue repair and reshaping are required, sometimes in multiple stages.
Before surgery, a patient goes through a consultation, including a discussion of anaesthesia options such as local numbing, spinal anaesthesia or general anaesthesia, depending on anxiety and personal preference. This will also determine the total cost of the procedure.
Surgery under general anaesthesia costs between Sh250,000 and Sh300,000, while spinal anaesthesia costs between Sh100,000 and Sh150,000.
The surgery takes about an hour for type one and two FGM cases. More complex repairs take longer, especially when reconstructing surrounding anatomy such as the clitoral hood and labia.
The primary aim, he explains, is to locate the remaining part of the clitoris and bring it forward.
“A reconstructed clitoris may not feel exactly the same, but some sensation and function is regained,” he says.
Recovery is often quick, with most women healing externally within two to three weeks. Internal healing takes longer, and swelling can last up to six weeks. Pain is generally minimal, although this varies from person to person.
O-Shot
Some women choose to enhance sensation through a cosmetic procedure known as the O-Shot (orgasm shot), an injection intended to improve stimulation.
“What we inject stimulates nerve growth,” says Dr Matwa. This add-on procedure costs between Sh40,000 and Sh120,000.
“We don’t get teenagers,” he says. “Women come after they’ve learned, questioned and made the choice for themselves,” adding that he performs four to five reconstructive surgeries a year.
Yet even as more women seek these surgeries, the stigma surrounding them makes it impossible to discuss openly with their mothers.
“All of us who’ve done it; my sisters and I, our friends; can never tell our mothers. My mother is old. She still believes in the female circumcision tradition. She even struggles with the fact that all of us have daughters and that we refuse to circumcise them. Now, imagine if we told her we’ve had reconstruction surgery to undo a cultural practice—that would be the worst. Even if FGM ends with our generation, it’s still taboo to talk about reconstruction, or even sex and women’s bodies,” Safia says.
Are there follow-up check-ups, like with other surgeries?
“No, no,” she says. “However, there’s this thing I’m planning to do. Since I am, you know, a normal woman, for lack of a better word, I’m looking at ways to make myself feel even better. One of the things my surgeon mentioned, and something I’ve seen other women do, is called the O-Shot (the orgasm shot). It’s supposed to enhance relations,” says the mother of two.
Follow our WhatsApp channel for breaking news updates and more stories like this.